|
|
|
|
|
|
|
|
|
|
HOW DO I GET STARTED WITH PATHWAY PLUS REIMBURSEMENT SUPPORT? |
|
||||
|
|
|
|
|
|
|
|
|
|
Download and print the Request Form found on this page for the product you are recommending to your patient. (Use the General form for products not listed) |
|
Complete all sections (or have your patient complete the Patient Information and Insurance Information sections of the form) and sign and date the Authorization to Share Medical Information page. |
|
Have your healthcare provider complete the remaining sections and fax the completed form to 855-752-9885 | |
|
|
|
|
|

|
||||||||
|
|
|

|
|
|
||||||||
|
|
|
|
|
|
||||||||

|
|
DOWNLOAD THE REQUEST FORM BELOW TO INITIATE
A PATHWAY PLUS SERVICE OR VISIT THE WEBSITE FOR MORE INFORMATION ABOUT THE PRODUCT. |
|
|
||||||||
|
|
|
|
|
|||||||||
|
|
|
|
||||||||||
|
|
|
|
|
|||||||||
|
|
|
|
||||||||||
|
|
|
|
|
|||||||||
|
||||||||||||

|
|||
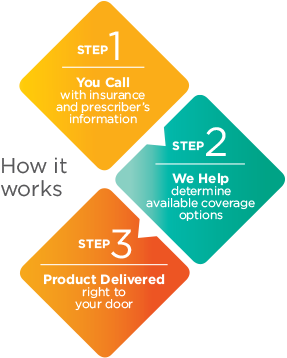
DOWNLOADS AND RESOURCESHow PATHWAY PLUS guides patients and providers through the reimbursement process: |
|||

|
The doctor examines and recommends a treatment plan to the patient(s). | ||

|
The doctor contacts PATHWAY PLUS to help confirm the patient’s healthcare coverage for the recommended Abbott Nutrition product. PATHWAY PLUS will need certain information in order to complete this service. (See below for the request forms you may need).
|
||

|
PATHWAY PLUS provides a written summary of benefits to the doctor and verbally relays coverage results and any out-of-pockets costs to the patient.
|
||
What information you will need to use PATHWAY PLUS:
Prior Authorization TipsPrior authorization requirements vary among health care plans. We have listed below some of the forms and documents you might need for a health plan to obtain prior authorization. This list does not guarantee prior authorization approval.
|
|||